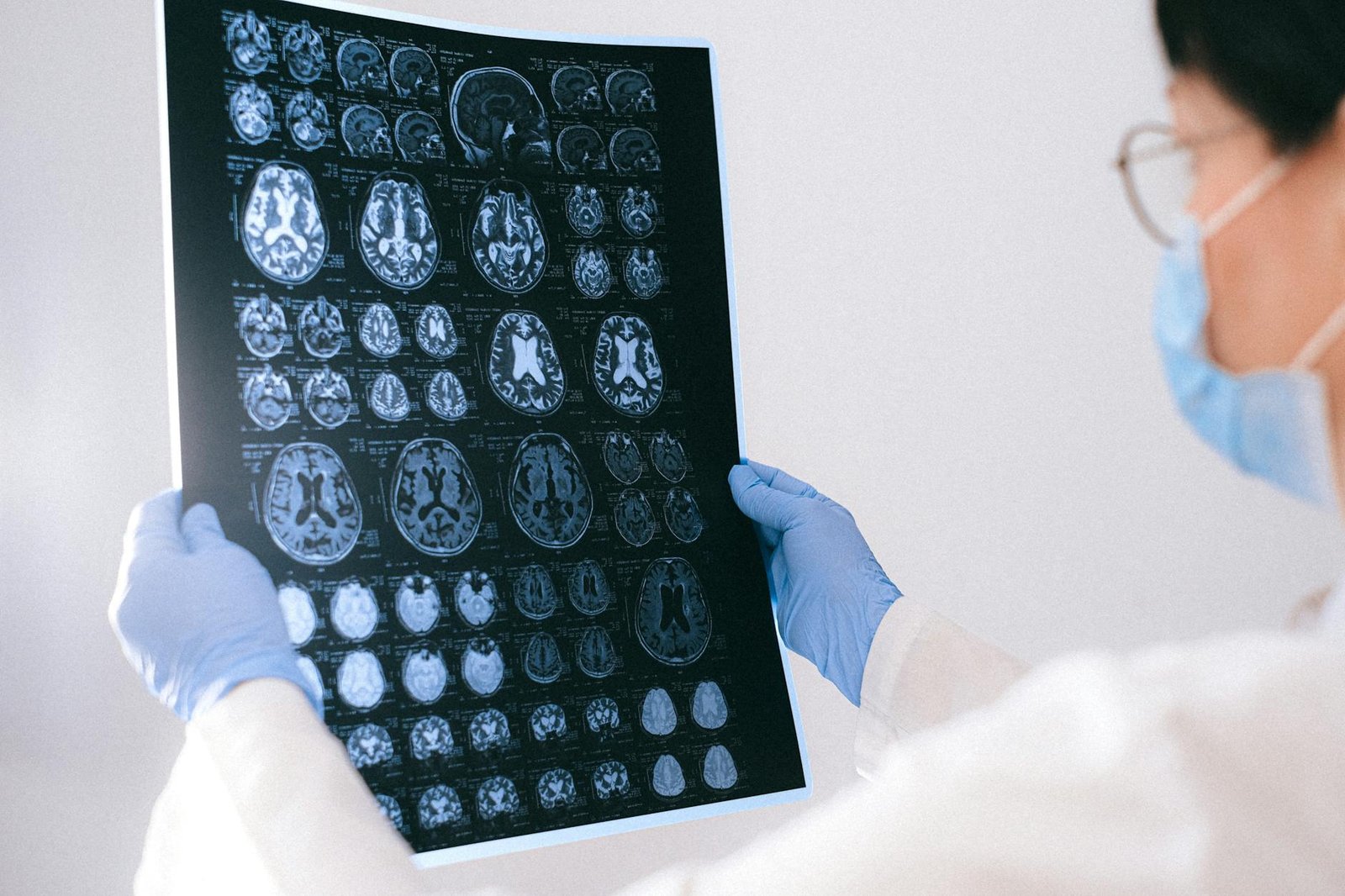
A significant milestone has been reached in the rapidly evolving world of health technology. A novel artificial intelligence healthcare platform has secured Fast-Track Designation from the U.S. Food and Drug Administration, often simply called the FDA, for its innovative diagnostic tool. This move, announced earlier this month, signals a pivotal moment for integrating advanced AI into the bedrock of medical diagnostics, promising to accelerate its development and review.
The platform, known as “MediMind AI,” developed by Veridian HealthTech, is specifically designed to identify early markers for a notoriously elusive neurodegenerative condition. Think about it: a system that can flag potential issues before symptoms even fully manifest, potentially changing countless lives. This isn’t just another incremental update; it’s a jump forward.
This Fast-Track status isn’t granted lightly. It means the FDA recognizes the diagnostic’s potential to address an unmet medical need and provides a pathway for more frequent communication and a potentially expedited review process. For a field as critical and heavily regulated as healthcare, such an endorsement from the FDA is a powerful statement about the technology’s promise. We’re talking about a future where diagnoses could be faster, more accurate, and more accessible than ever before, all thanks to the relentless march of artificial intelligence in healthcare.
Key Takeaways
- Veridian HealthTech’s MediMind AI platform received FDA Fast-Track Designation for a novel neurodegenerative diagnostic.
- Fast-Track status signifies the diagnostic addresses an unmet medical need and facilitates expedited development and review.
- The AI aims to detect early biomarkers for a currently elusive neurodegenerative condition, potentially transforming early intervention.
- This approval underscores the growing acceptance and regulatory confidence in artificial intelligence applications in medical diagnostics.
- Ethical considerations, data privacy, and algorithmic bias remain crucial discussion points as AI integration expands in health technology.
Table of Contents
- A New Era for Medical Diagnostics with AI
- Understanding FDA Fast-Track Designation
- The Technology Behind MediMind AI
- How AI is Transforming Healthcare Diagnostics
- Regulatory Challenges and Ethical Considerations
- The Future Outlook for AI in Medicine
- Frequently Asked Questions About AI in Healthcare
A New Era for Medical Diagnostics with AI
The FDA’s decision regarding MediMind AI heralds what many believe is a new era for medical diagnostics. For years, the promise of artificial intelligence in healthcare has been discussed in academic papers and at industry conferences. But here’ the thing: actual, tangible regulatory approval brings these discussions into the realm of practical application. It validates years of research and development, showing that AI can indeed move beyond theoretical models to offer concrete solutions in clinical settings.
This approval comes at a time when healthcare systems globally are grappling with increasing demands and the need for more efficient, accurate diagnostic tools. Manual diagnostic processes, while foundational, can sometimes be slow and prone to human variability. AI, with its capacity for rapid data analysis and pattern recognition, offers a powerful complement. The ability to process vast amounts of medical data — imaging, genetic information, patient histories — at speeds human clinicians simply cannot match, is where the real power lies.
We’ve seen how quickly technology can reshape industries. Just look at the progress in areas like autonomous vehicles or even advanced climate modeling. Healthcare, historically slower to adopt radical technological shifts due to stringent safety and efficacy requirements, is now demonstrating a readiness for change. This isn’t about replacing doctors; it’ about equipping them with unprecedented tools.
The Impact on Patient Outcomes
Ultimately, the true measure of any medical innovation is its impact on patient outcomes. For a neurodegenerative condition that often progresses silently for years before diagnosis, early detection can be paramount. It can open windows for interventions that might slow disease progression, improve quality of life, or allow patients and their families to plan more effectively. This is where the “novel” aspect of MediMind AI truly shines.
Consider the potential: fewer misdiagnoses, earlier treatment initiation, and a more personalized approach to care. These aren’ small details. They are shifts that could fundamentally alter the trajectory of diseases previously thought untreatable or unmanageable in their early stages. The FDA’ Fast-Track decision implicitly acknowledges this profound potential, prioritizing its journey to patients who desperately need better options.
Understanding FDA Fast-Track Designation
For those outside the pharmaceutical and medical device industries, the term “Fast-Track Designation” might sound like a simple shortcut. But it’ anything but. It’ a formal process, established by Congress in 1992, designed to facilitate the development and expedite the review of new drugs and biologics to treat serious conditions and fill an unmet medical need. The FDA extends this logic to novel medical devices and diagnostics that meet similar criteria.
What does it truly mean for a company like Veridian HealthTech? It means regular, often weekly, meetings with FDA officials to discuss development plans, clinical trial designs, and data collection. It can also lead to eligibility for other expedited review programs, such as Accelerated Approval, Priority Review, and even Rolling Review, where the company can submit portions of its application for review as they are completed, rather than waiting for the entire package.
The intent is clear: when there’ a critical health problem with no good solutions, the FDA wants to get promising therapies and diagnostics to patients as quickly and safely as possible. It’ a rigorous process, make no mistake, but one designed for speed and efficiency in areas of high medical urgency. This isn’ some kind of regulatory bypass; it’ a dedicated, streamlined highway.
Distinguishing Fast-Track from Other FDA Pathways
The FDA has several pathways for expedited review, each with specific criteria. It’ easy to get them confused. Fast-Track, as we’ discussed, focuses on meeting an unmet medical need for a serious condition. Priority Review shortens the FDA’ review clock. Breakthrough Therapy Designation offers an even more intensive version of Fast-Track benefits for drugs that show substantial improvement over existing therapies. And then there’ Accelerated Approval, which allows for approval based on a surrogate endpoint likely to predict clinical benefit.
MediMind AI securing Fast-Track is significant because it recognizes the inherent difficulty in diagnosing this particular neurodegenerative condition and acknowledges the AI’ potential to make a genuine difference. It’ a formal recognition of the clinical importance of this specific artificial intelligence in healthcare application.
| FDA Designation | Primary Criterion | Key Benefit |
|---|---|---|
| Fast-Track | Treats serious condition and fills unmet medical need. | Frequent FDA communication, potential for expedited review (e.g., Rolling Review). |
| Breakthrough Therapy | Preliminary clinical evidence indicates substantial improvement over existing therapy. | Intensive guidance, organizational commitment, all Fast-Track features. |
| Priority Review | Significantly improves safety or effectiveness of treatment for serious conditions. | Shortens FDA review timeline (e.g., from 10 to 6 months). |
| Accelerated Approval | Serious conditions where product provides meaningful therapeutic advantage over existing treatments, often based on surrogate endpoint. | Approval based on surrogate endpoints, continued verification required. |
The Technology Behind MediMind AI
So, what exactly makes MediMind AI tick? At its core, it’ a sophisticated machine learning platform trained on an immense dataset of anonymized patient records, medical images, genetic sequences, and clinical outcomes. The goal is to identify subtle patterns and correlations that human perception might miss or find too complex to synthesize efficiently. This is the essence of modern artificial intelligence in medical diagnostics.
The platform utilizes deep learning algorithms, a subset of machine learning, which are particularly adept at image recognition and pattern identification. Researchers at Veridian HealthTech have reportedly fed the system millions of data points related to the neurodegenerative condition, allowing it to “learn” the intricate signatures of early disease presence. This kind of robust training is critical for any AI system meant for clinical use, requiring meticulous curation and validation of data.
The diagnostic works by analyzing a combination of input data, potentially including high-resolution brain scans, blood biomarker profiles, and even subtle changes in patient cognitive test results over time. It’ not just looking for one smoking gun; it’ constructing a holistic probabilistic model. And that’ quite powerful. One tool that stands out for robust data handling in research settings is the Dell Precision 7920 Tower Workstation, often favored by data scientists for its processing capabilities when dealing with large medical datasets.
Accuracy and Validation in Clinical Trials
The path to FDA Fast-Track status, and ultimately full approval, is paved with rigorous clinical trials. Veridian HealthTech presented compelling data demonstrating the platform’ accuracy in identifying the neurodegenerative condition at stages earlier than conventional methods allowed. The specificity and sensitivity metrics reported were impressive, especially considering the early-stage detection capabilities.
Independent validation studies were also crucial, ensuring that the AI’ performance wasn’ just robust within Veridian’ own controlled environment, but also across different clinical settings and patient populations. This level of scrutiny is paramount to building trust in AI diagnostics, particularly when previous concerns about “black box” biases have arisen. Remember the FDA Halts AI Diagnostic Rollout Over ‘Black Box’ Bias news? That’ exactly why transparency and rigorous validation are non-negotiable.
For individuals interested in understanding the foundational principles of how these advanced systems operate, a good starting point could be “Machine Learning for Healthcare Professionals” by Emily G. Smith, which offers a clear overview without getting bogged down in overly technical jargon.
How AI is Transforming Healthcare Diagnostics
The approval of MediMind AI isn’ an isolated incident; it’ part of a broader trend of artificial intelligence reshaping health technology. Beyond neurodegenerative diseases, AI is making inroads in numerous diagnostic areas.
For instance, in radiology, AI algorithms can analyze X-rays, CT scans, and MRIs with remarkable speed and often with accuracy comparable to, or even exceeding, human experts, particularly in detecting subtle anomalies. In pathology, AI can assist in analyzing tissue biopsies for cancer detection and grading. Even in ophthalmology, AI tools are now capable of screening for diabetic retinopathy and other eye conditions from retinal images. The sheer breadth of application is staggering.
Efficiency and Accessibility Gains
One of the most immediate benefits of this shift towards AI-powered diagnostics is the potential for increased efficiency. Automating parts of the diagnostic process can free up clinicians to focus on complex cases and direct patient care. It means faster turnaround times for results, which can be critical for patient anxiety and treatment planning.
And then there’ accessibility. Imagine a world where specialized diagnostic capabilities, currently confined to major urban medical centers, could be deployed in remote or underserved areas through AI-powered portable devices. This is not science fiction; it’ already beginning to happen. For example, some point-of-care ultrasound devices now incorporate AI to guide users and interpret images. Many readers swear by the Philips Lumify handheld ultrasound for its portability and image quality in various clinical settings.
Such advancements hold particular promise for global health initiatives, allowing for early screening and diagnosis in populations that historically lack access to specialized medical expertise. It reduces the dependency on a limited pool of highly trained specialists, democratizing access to crucial diagnostic information. This is why artificial intelligence in medicine is so exciting.
Regulatory Challenges and Ethical Considerations
While the excitement around MediMind AI and similar innovations is palpable, it’ vital to acknowledge the inherent challenges. Regulatory bodies like the FDA are navigating uncharted territory. How do you regulate an algorithm that “learns” and adapts? The traditional regulatory framework, built around static medical devices, often struggles with the dynamic nature of advanced AI models.
The issue of algorithmic bias is another major concern. If the AI is trained on data primarily from one demographic group, it might perform poorly, or even incorrectly, when applied to patients from underrepresented populations. This can exacerbate existing health disparities. Robust data diversity and continuous monitoring are essential to mitigate these risks. As we’ explored in the past, Major Tech Firms Pause Generative AI Amid Ethical Calls, highlighting these very ethical dilemmas.
Data Privacy and Security
The massive datasets required to train powerful AI models in healthcare raise significant data privacy and security questions. Protecting sensitive patient information is non-negotiable. Strong encryption, anonymization techniques, and stringent access controls are paramount. A breach in a healthcare AI platform could have devastating consequences, not just for individuals but for public trust in health technology itself.
And it’ not just about protection. It’ about patient consent. Do patients fully understand how their data will be used when contributing to these vast AI training pools? Clear, transparent communication and robust ethical guidelines are necessary to ensure that individuals maintain control over their personal health information. The line between innovation and intrusion can be very thin, indeed.
It brings to mind discussions around other evolving health tech, like Smart Contact Lenses with AR & Health Diagnostics: Future Vision or Privacy Nightmare?, where data privacy is a central concern from the outset.
The Future Outlook for AI in Medicine
The FDA’ Fast-Track approval for MediMind AI is more than just a win for one company; it’ a positive indicator for the broader trajectory of artificial intelligence in healthcare. It signals a maturation of the field, moving from speculative potential to concrete, regulator-approved solutions. The momentum is undeniable.
We can expect to see an accelerating pace of innovation in medical diagnostics. More AI platforms will seek and likely receive similar designations as their efficacy and safety profiles are rigorously demonstrated. This will lead to a richer ecosystem of tools, each addressing specific unmet needs across a spectrum of diseases, from oncology to cardiology to mental health.
But the journey isn’ without its continued challenges. Integration into existing healthcare workflows, training clinicians to effectively use and trust these tools, and continuously updating and validating AI models will require ongoing effort. It will also demand sustained collaboration between tech developers, medical professionals, patients, and regulatory bodies.
Patient Empowerment and Personalized Care
Ultimately, the overarching goal of integrating advanced health technology like AI into medicine is to improve patient lives. Better diagnostics mean more informed decisions, more personalized treatment plans, and potentially, a greater sense of control for patients over their health journey. Imagine receiving an early warning for a condition, accompanied by a clear, data-driven explanation and a personalized action plan. That’ the promise of this technology.
This isn’ just about algorithms; it’ about human flourishing. When artificial intelligence can help us see what was previously invisible, when it can offer hope where there was once uncertainty, that’ when we truly harness its transformative power. The MediMind AI approval is a strong step in that direction, pushing the boundaries of what’ possible in medical diagnostics.
Many individuals are also exploring personal health monitoring devices to track their wellness metrics proactively. A highly-rated option for this is the Fitbit Sense 2 Advanced Health Smartwatch, which offers continuous heart rate tracking, stress management tools, and sleep monitoring, providing valuable personal data that could one day integrate with advanced AI diagnostic systems for even more comprehensive health insights.
Frequently Asked Questions About AI in Healthcare
What does FDA Fast-Track Approval mean for an AI diagnostic?
FDA Fast-Track Approval means the diagnostic addresses a serious condition and fulfills an unmet medical need. This designation facilitates more frequent communication with the FDA and allows for an expedited review process, potentially including options like rolling review, to bring the technology to patients faster.
Is AI in medical diagnostics safe and accurate?
Regulatory bodies like the FDA require rigorous testing and validation of AI diagnostics to ensure their safety and accuracy. While AI offers immense potential for precision and efficiency, robust clinical trials and continuous monitoring are essential to confirm performance and mitigate risks such as algorithmic bias.
Will AI replace doctors in diagnosing diseases?
It’s highly unlikely that AI will replace doctors. Instead, AI is envisioned as a powerful tool that augments clinicians’ capabilities, providing faster, more precise analyses of complex data. It aims to assist doctors in making more informed decisions, freeing up their time for direct patient care and complex problem-solving, rather than acting as a substitute.
How does AI learn to diagnose diseases?
AI learns to diagnose diseases by being trained on vast datasets of medical information, including patient records, imaging scans, genetic data, and laboratory results. Advanced machine learning algorithms, particularly deep learning, identify subtle patterns and correlations within this data that are indicative of specific conditions, allowing the AI to “learn” how to detect these patterns in new patient data.
What are the main ethical concerns with AI in healthcare?
Key ethical concerns include algorithmic bias, where AI systems might perform differently across diverse patient populations if not trained on representative data. Data privacy and security are also paramount, as AI requires access to sensitive patient information. Transparency in how AI makes decisions, often called the “black box” problem, is another significant ethical consideration.
How will AI diagnostics impact healthcare costs?
The impact on healthcare costs is complex and could vary. Initially, development and integration costs for AI diagnostics might be high. However, in the long term, AI could reduce costs by enabling earlier diagnosis, preventing advanced disease, optimizing treatment plans, and improving efficiency in clinical workflows. It’ a balance of upfront investment versus long-term savings and improved outcomes.
What types of diseases can AI currently diagnose?
AI is currently demonstrating diagnostic capabilities across a wide range of diseases. This includes detecting cancers from medical images and pathology slides, identifying eye diseases like diabetic retinopathy, screening for cardiovascular conditions, and, as with MediMind AI, recognizing early markers of neurodegenerative disorders. The scope continues to expand rapidly as technology advances.
The FDA’ Fast-Track approval for Veridian HealthTech’ MediMind AI is a landmark event. It underscores a fundamental shift in how medical diagnostics are developed, evaluated, and ultimately deployed. This isn’ just about a single product; it’ about the accelerating integration of artificial intelligence into the very fabric of healthcare. While challenges around ethics, data privacy, and regulatory adaptation will persist, the clear trajectory is towards a future where AI empowers clinicians with unparalleled tools for earlier, more accurate diagnoses, paving the way for significantly improved patient outcomes. The journey is certainly far from over, but this step undeniably marks a powerful stride forward for health technology.
TRENDING: Smart Contact Lenses with AR & Health Diagnostics: Future Vision or Privacy Nightmare?
Download the new game Guess The Celebrity Quiz and check how well you know your idols
Always be up to date with the news and follow the trends!
 Support our work by giving us a small donation
Support our work by giving us a small donation